Dry eye treatment
Comprehensive care to relieve dry eye symptoms
Summary of dry eye treatment
- Dry eye is a manageable eye condition
- Having treatment sooner than later helps avoid related eye problems
- First, we assess your dry eye
- Once we know the cause, we recommend a personalised treatment plan
- The prognosis for visual acuity in patients with dry eye syndrome is generally good
Dry eye treatment – An introduction
We see patients who suffer from dry eye syndrome on a daily basis. We have developed an approach with comprehensive care to relieve dry eye symptoms at different levels.
Dry eye management includes:
- The study of your profile,
- The quantification of the severity of the symptoms you feel,
- The complete ophthalmic examination,
- Lipiview ®, which makes it possible to measure the Meibomian attack as well as the analysis of the dynamics of the blinking.
Consequently, this approach allows us, in many cases, to recommend therapeutic management that provides relief of dry eye symptoms.
ENJOY LIFE WITHOUT CONTACTS OR GLASSES
CONTACT US TO FIND OUT IF YOUR EYES ARE SUITABLE FOR LASER EYE SURGERY
How do you know dry eye treatment is right for you?
TearScience® – An assessment of dry eye in 3 steps:
- You describe your symptoms in a quick questionnaire (sensations, disorders and more).
- A 3-minute, non-contact, pain-free examination with LipiView ®, the ocular surface interferometer, which allows observation of tear film and blink dynamics.
- We examine your eyelids to evaluate secretions (this examination is painless)
Finally, these three steps help us confirm the cause of your dry eye as:
- either a lipid deficiency, due to dysfunction of the Meibomian glands (86% of cases), or
- an aqueous deficiency, due to dysfunction of the lacrimal glands.
TAKE THE FIRST STEP TOWARDS BETTER VISION
FIND OUT IF YOUR EYES ARE SUITABLE FOR LASER VISION CORRECTION
Dry eye treatment – Further details
Our diagnostic and therapeutic approach
Four clinical team members will support you to conduct an overall analysis of your pathology.
Step 1
The assistant will welcome you and provide you with a SPEED questionnaire to complete in the waiting room as well as a file of information on the progress of the treatment, on the dry eye, its causes, and the possible therapies.
The Patient Questionnaire (SPEED: Standard Patient Evaluation of Eye Dryness) allows the patient to describe the symptoms they feel (dryness, a sensation of sand grains or itching, a sensation of pain, burning or tearing sensation, eye strain), their frequency and their severity. The maximum score you can obtain is 28. The categories are:
- SPEED = 0 no symptoms
- SPEED between 1 and 9 mild to moderate symptoms
- SPEED ≥ 10 Severe symptoms
Step 2
We work with a sophrologist, which is very useful for these patients whose pathology causes suffering which is almost permanent sometimes very disabling.
Indeed, sophrology is a science that studies human consciousness and aims to reinforce the balance between our emotions, our cognition and our behaviours. It allows a person to consolidate their physical and mental structures, and thus the management of psychosomatic manifestations. Once we confirm the diagnosis, we will involve the sophrologist.
Since the human being is an entity, sophrology proposes to focus on a specific need. According to a jointly established protocol, we design the patient’s approach after a complete a complete medical history. That allows us to precisely target the patient in all stages of their life, thus revealing the causes that lead to dry eye. This patient history makes it possible to take into account the factors that induce the establishment of this pathology. It is also important to highlight the notion of suffering that causes pain. When the patient establishes the correlation of the trigger, we can facilitate ophthalmological therapeutic management.
In this case, it is the patient who has been confronted with a significant emotional event. By developing the objective reality of the patient, it allows him to appreciate events as they are, to develop more realism and efficiency in action. The reinforcement of their positive action directed towards their body or their mind leads with the necessary treatment to have a positive repercussion on his whole being.
Step 3
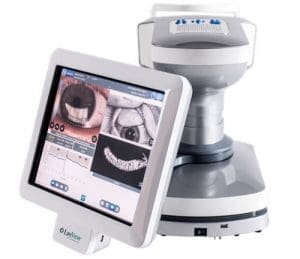 The orthoptist then takes charge of the patient for complementary examinations with the Lipiview® (fig 1). LipiView® is a non-invasive ophthalmic imaging device that captures, archives and stores digital images. It a few minutes, it analyses the tear film, blinking and Meibomian glands.
The orthoptist then takes charge of the patient for complementary examinations with the Lipiview® (fig 1). LipiView® is a non-invasive ophthalmic imaging device that captures, archives and stores digital images. It a few minutes, it analyses the tear film, blinking and Meibomian glands.
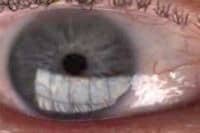
- The analysis of the tear film quality and the estimation of the thickness of the lipid layer measured in nanometers (FIG. 2) is obtained by specular reflection interferometry.
The colourimetry is uniformly grey when the lipid layer is absent or less than 60 nanometers. When the interference fringes are stained with gradual colour changes: the thickness of the lipid film is normal, that is to say, higher than 100 nm. The examination is dynamic and we analyze by video stretching the tear film on the corneal surface after each blink.
- This device has the advantage of restoring (image by image) the film of the eyelid blinking which allows the analysis of blinking: whether it has a regular rhythm or not, its frequency – about one blink every five to six seconds – and especially the count of the incomplete blinks. When the lipid layer is abnormal or invisible, the evaporation rate of the tear film increases by a factor of four. Patients with a thinner lipid layer should blink more wholly and frequently to renew the lipid film and prevent corneal dryness. In the opposite case blinking exercises must be prescribed.
- Finally, LipiView® provides dynamic images of the Meibomian glands (Fig 3)
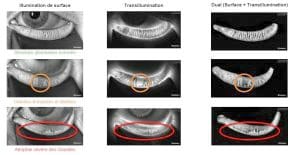 by the combination of an infrared surface meibography and infrared transillumination of the lower eyelids. This combination is made possible by the use of an infrared transilluminator whose light intensity adapts to the thickness of the eyelids to ensure a uniform visualization of the glandular structures. We can thus evaluate the presence of meibomian plugs and the level of atrophy.
by the combination of an infrared surface meibography and infrared transillumination of the lower eyelids. This combination is made possible by the use of an infrared transilluminator whose light intensity adapts to the thickness of the eyelids to ensure a uniform visualization of the glandular structures. We can thus evaluate the presence of meibomian plugs and the level of atrophy.
Step 4
We orient the ophthalmological examination according to the results of previous tests. The examination must be comprehensive and focused on the analysis of the eyelids, conjunctiva, tear film and cornea. The evaluation of Meibomian gland secretion (MGE: Meibomius tassels evaluation) refines the diagnosis. We’ve standardised this step thanks to the use of a new instrument that allows the application of constant pressure at the free edge in front of 5 Meibomian glands. We analyse the expression of the glands nasally, centrally and temporally in each lower eyelid. (Fig 4) Meibomian secretion usually is fluid and transparent. According to the severity of the dysfunction of the Meibomian glands, it can be greasy fluid, slightly cloudy or opaque, and thick.
Meibomian secretion usually is fluid and transparent. According to the severity of the dysfunction of the Meibomian glands, it can be greasy fluid, slightly cloudy or opaque, and thick.
Once we confirm the diagnosis and assess the severity of the impairment, we propose treatment which can be:
- We can combine a local treatment based on lubricating eye drops according to their preferred action
- Local anti-inflammatory treatment. Depending on the case, we may offer
- corticosteroid eye drops,
- nonsteroidal anti-inflammatory drugs,
- antibiotics with anti-inflammatory activity,
- calcineurin inhibitors or a newborn glycyrrhizin,
- a new molecule available since January 2016 in the form of eye drops,
- Kéradrop®.
- 1 drop in the morning and evening for 3 months has an anti-inflammatory action that is equivalent to dexamethasone without side effects.
- Eyelid hygiene
- Blinking exercises
- We can supplement these treatments with two technologies that have proven effectiveness:
Lipiflow ®
Lipiflow ® allows eyelid hygiene targeted in time and temperature. It uses advanced technology and components to control the heat applied to the inner surface of the eyelids and perform rhythmic massage of the outer surface of the eyelids to facilitate lipid production of the cystic Meibomian glands.
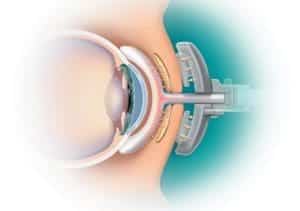
- The device comprises of 2 parts. An external eyecup (Eye Cup) in contact with the upper and lower eyelids.It contains a flexible and flexible pouch that inflates with intermittent air and performs a controlled massage of the eyelids. An inner part (Lid warmer) resembling a large scleral glass 24 mm in diameter, whose periphery rests on the bulbar conjunctiva, which is molded on the inner side of the eyelids while remaining at a distance from the cornea.The heat emitted by this part is of 42,5 °C which makes it possible to melt the material obstructing the glands by the interior, without damaging the glands themselves. (Fig 5 ab). It allows simultaneous treatment of the glands of the lower and upper eyelids. The procedure lasts about 12 minutes and we perform it in the doctor’s office. The treatment is not painful and is rather pleasant for the patient. It causes a moderate conjunctival hyperemia a few hours but no other side effect. It is indicated in case of obstruction of most Meibomian glands when the MGE is less than 5.
- Pulsed Light E-Eye. The E-EYE apparatus (FIG. 6) is a polychromatic pulsed light generator capable of producing calibrated and
 homogeneous light pulse sequences. The emitted light called “cold light” stimulates the Meibomius glands by applying 5 spots at the inferior and temporal orbital rim along the parasympathetic terminations (Fig. 7). The treatment is non-invasive and completely painless. 3 or 4 sessions spaced 15 days and then 1 month are necessary. This treatment is indicated in addition to Lipiflow® or only if the majority of Meibomian glands are not blocked.
homogeneous light pulse sequences. The emitted light called “cold light” stimulates the Meibomius glands by applying 5 spots at the inferior and temporal orbital rim along the parasympathetic terminations (Fig. 7). The treatment is non-invasive and completely painless. 3 or 4 sessions spaced 15 days and then 1 month are necessary. This treatment is indicated in addition to Lipiflow® or only if the majority of Meibomian glands are not blocked.


Conclusion
Dry eye is a complex pathology whose causes are multifactorial. The diagnostic approach must be comprehensive for better diagnostic and therapeutic management.

DISCOVER A NEW LIFE FREE FROM THE HASSLE OF GLASSES OR CONTACTS
CALL TO FIND OUT IF YOU CAN BENEFIT FROM LASER EYE SURGERY
TÉMOIGNAGES

“Le jour de l’intervention, je n’ai ressenti aucune gêne et aucune douleur. Après 2 h de repos j’ai pu reprendre mes activités tout à fait normalement. Deux jour après l’intervention il ne subsiste aucune gêne. Je tenais également à insister sur le fait que, contrairement aux idées reçues, ce n’est pas une intervention réservée aux personnes jeunes. J’ai 59 ans et c’est une totale réussite.”

“Le Docteur Albou-Ganem m’a opérée de la presbytie il y a un an, et je suis très heureuse du résultat, plus besoin de lunettes pour lire, même ma vue de loin est bonne. C’est un vrai soulagement pour moi, car j’ai hésité pendant un moment avant de sauter le pas, difficile de prendre une telle décision.”

“Après une opération rapide et sans douleur j’ai quasiment immédiatement remarqué une nette amélioration de ma vue de près et de loin. Au fil des semaines cela n’a fait que se confirmer et je n’ai jamais reporté mes lunettes depuis! Je ressens une telle liberté dans ma vie de tous les jours ainsi qu’une impression d’avoir rajeuni que je recommande à toute personne de le faire sans hésitation si cela leur est possible!”

“Docteur Catherine Albou-Ganem l’a immédiatement dissipée. Contact et confiance se sont installés immédiatement. Ses explications ont été claires, précises et je peux dire que le Jour J de l’opération, j’y suis allé les yeux fermés! Pour les rouvrir quelques heures plus tard avec la vue parfaite d’un homme de 30 ans!”

“L’opération a été un franc succès. J’ai maintenant 10/10e, sachant qu’auparavant j’avais une assez forte myopie (-5 et et -4,5) et un léger astigmatisme.”

“Vous m’avez opérée il y a maintenant plus de deux ans. A part pour conduire et regarder la télévision, et encore… je n’ai plus besoin de lunettes, moi qui n’ai jamais rien vu… Il m’a fallu plusieurs mois pour que ma vue s’adapte. Je tenais donc à vous remercier de cette opération qui a changé ma vie! Plus d’ulcères douloureux dus aux lentilles et la possibilité d’ouvrir les yeux sous l’eau et d’admirer les jolis poissons!”
We have replaced the images of real patients who provided these testimonials to protect their privacy.
DISCOVER WHETHER YOU ARE SUITABLE FOR LASER EYE SURGERY
FIND OUT IF YOU CAN BE FREE FROM YOUR GLASSES OR CONTACT LENSES
AFFILIATIONS & MEMBERSHIPS
We are pleased to be associated with the following organisations
About the author
Doctor Catherine Albou-Ganem
Consultant Ophthalmic Surgeon
I am Catherine Albou-Ganem and I am an ophthalmic surgeon brought up in a family of ophthalmologists. I had a passion for ‘the eye’ and ‘the vision’ from my childhood. This was the subject of my first presentation at school.
Today, I share my refractive surgery activity between the hospital and the private sector.
I am proud to have contributed to the development of new laser refractive surgery techniques that can correct vision defects with accurate, effective and safe results when respecting the indications.
 Skip to content
Skip to content



 The colourimetry is uniformly grey when the lipid layer is absent or less than 60 nanometers. When the interference fringes are stained with gradual colour changes: the thickness of the lipid film is normal, that is to say, higher than 100 nm. The examination is dynamic and we analyze by video stretching the tear film on the corneal surface after each blink.
The colourimetry is uniformly grey when the lipid layer is absent or less than 60 nanometers. When the interference fringes are stained with gradual colour changes: the thickness of the lipid film is normal, that is to say, higher than 100 nm. The examination is dynamic and we analyze by video stretching the tear film on the corneal surface after each blink.